Mothers
Digital NST Monitoring vs Traditional Methods: What Hospitals Should Choose?
Feb 23 • 4 min read

Table of Content
Understanding the Nonstress Test for Pregnancy
What Is Traditional NST Monitoring?
Limitations Observed in Practice
What Is Digital NST Monitoring?
Digital NST Monitoring vs Traditional Methods: A Clinical Comparison
Clinical Advantages of
Improved Real-Time Oversight
Faster Clinical Escalation
Secure Data Archiving
Workflow Efficiency
Cost Considerations: Short- Term vs Long- Term Value
When Might Traditional NST Still Be Suitable?
The Role of Wireless and Portable
Evidence and Clinical Oversight
Conclusion: What Should Hospitals Choose?
The Nonstress Test (NST) remains one of the most widely used antenatal surveillance tools for assessing fetal well-being. As high-risk pregnancies increase and obstetric units manage higher patient loads, hospitals are re-evaluating whether traditional paper-based NST systems are sufficient or if digital NST monitoring offers a safer, more efficient alternative.
For decades, conventional bedside NST machines have supported fetal heart rate (FHR) and uterine contraction monitoring. However, advancements in wireless CTG machines, Bluetooth-enabled fetal monitoring systems, and centralized digital platforms are transforming how obstetric teams interpret and respond to fetal data.
This article provides an evidence-informed, clinician-focused comparison to help hospitals determine which system best supports maternal–fetal outcomes, workflow efficiency, and long-term scalability.
Understanding the Nonstress Test for Pregnancy
A Nonstress Test for Pregnancy evaluates fetal heart rate accelerations in response to fetal movements. It typically involves:
Continuous fetal heart rate monitoring
Simultaneous uterine contraction monitoring
Interpretation of baseline variability, accelerations, and decelerations
NSTs are recommended in cases such as:
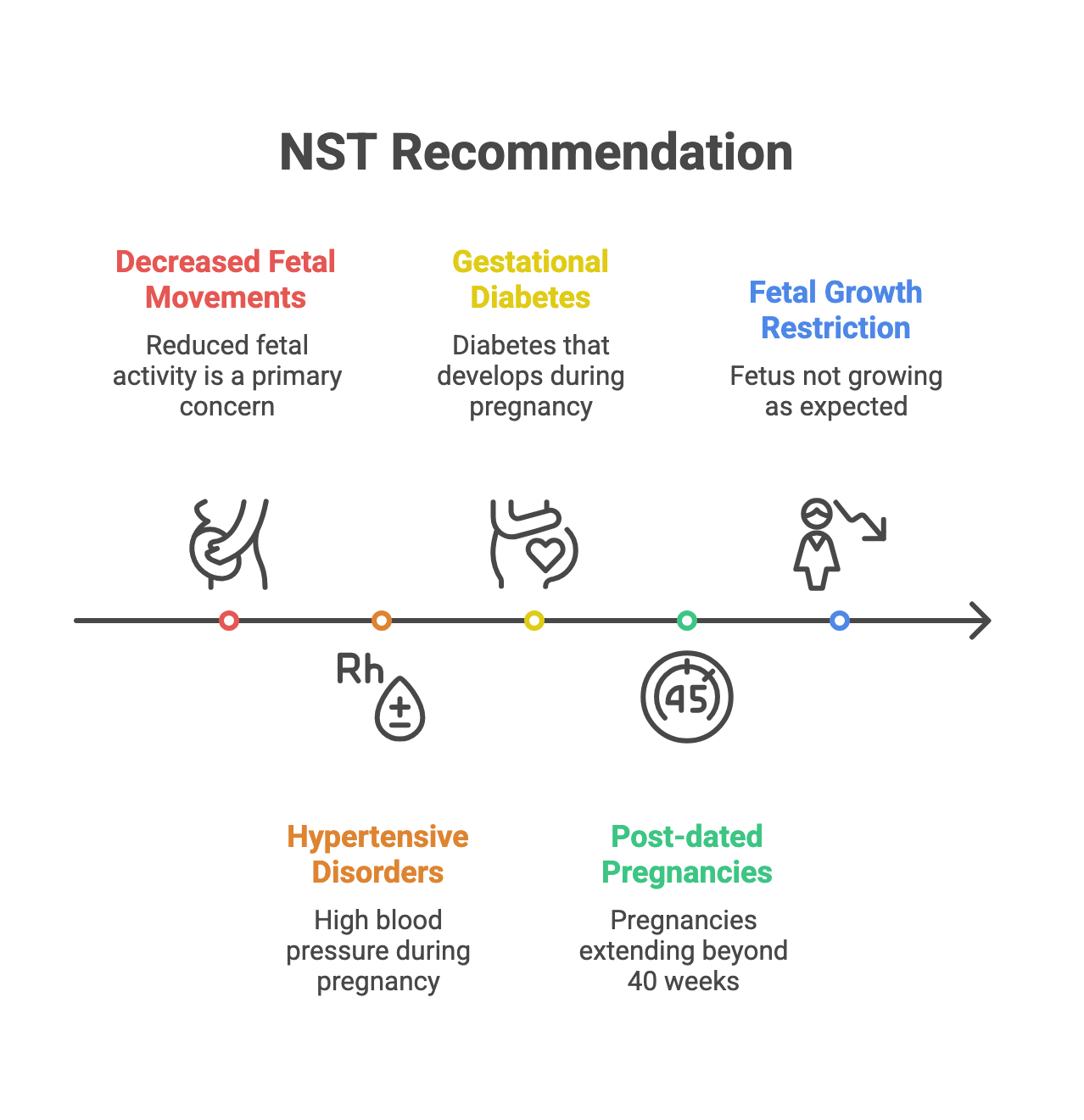
Decreased fetal movements
Hypertensive disorders
Gestational diabetes
Post-dated pregnancies
Fetal growth restriction
Traditionally performed in hospitals using cardiotocography (CTG), the NST remains a cornerstone of third-trimester fetal surveillance.
What Is Traditional NST Monitoring?
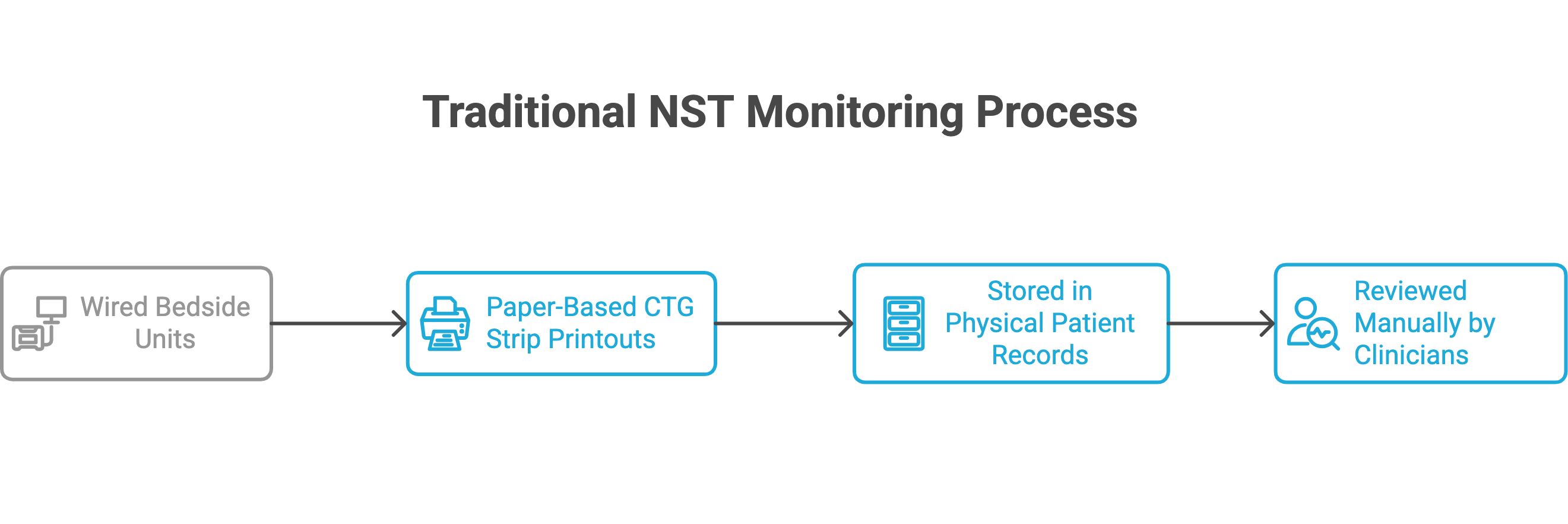
Traditional NST systems are typically:
Wired bedside units
Dependent on paper-based CTG strip printouts
Stored in physical patient records
Reviewed manually by clinicians
Limitations Observed in Practice
From a clinical operations perspective, hospitals often encounter:
Manual storage and retrieval challenges
Risk of paper loss or deterioration
Limited remote supervision
Reduced visibility in high-load labor rooms
Delayed escalation in centralized facilities
While traditional NST machines are reliable, their workflow constraints become evident in tertiary care and high-volume obstetric units.
What Is Digital NST Monitoring?
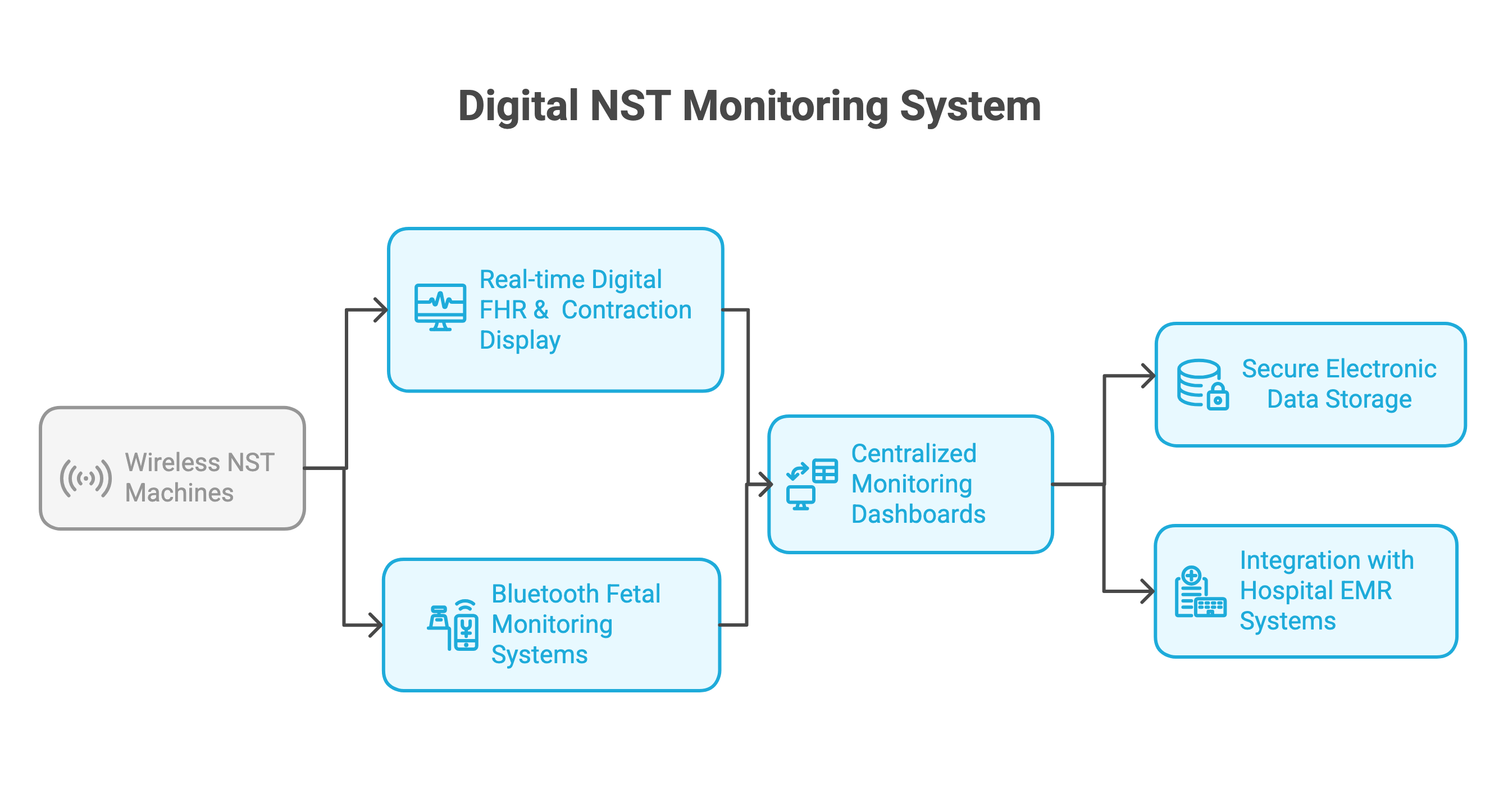
Digital NST monitoring systems integrate:
Wireless NST machines
Real-time digital FHR & contraction display
Bluetooth fetal monitoring systems
Centralized monitoring dashboards
Secure electronic data storage
Integration with hospital EMR systems
These systems function as part of a broader remote pregnancy monitoring ecosystem, improving accessibility and decision-making speed.
Digital NST Monitoring vs Traditional Methods: A Clinical Comparison
From an operational standpoint, digital systems enhance clinical visibility across multiple beds simultaneously.
Clinical Advantages of Digital NST Monitoring for Hospitals
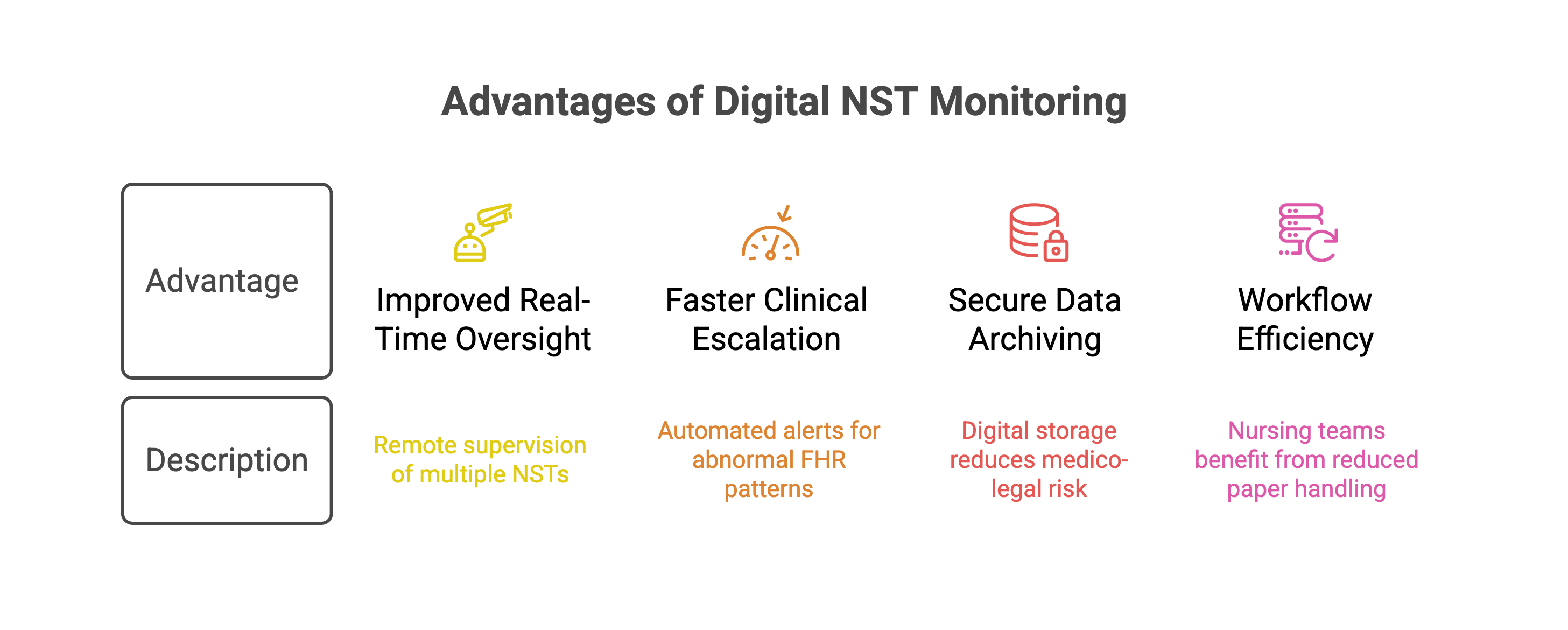
In high-volume obstetric settings, timely interpretation and coordinated response are critical to fetal safety. Digital NST monitoring systems are designed not only to capture data, but to enhance clinical visibility, documentation integrity, and workflow efficiency across maternity units.
Improved Real-Time Oversight
A centralized system allows senior obstetricians to supervise multiple NSTs remotely, especially useful in:
Busy maternity wards
Peripheral units connected to tertiary centers
Teaching hospitals
Faster Clinical Escalation
With automated alerts for abnormal FHR patterns, digital systems may support earlier intervention in cases of:
Prolonged decelerations
Reduced variability
Non-reactive NST patterns
Secure Data Archiving
Digital storage reduces medico-legal risk associated with:
Lost CTG strips
Faded thermal printouts
Documentation gaps
Workflow Efficiency
Nursing teams benefit from:
Reduced paper handling
Simplified documentation
Improved mobility with portable fetal monitoring devices
Cost Considerations: Short- Term vs Long- Term Value
While traditional NST systems often involve lower upfront costs, hospitals must evaluate:
Paper and maintenance expenses
Storage infrastructure
Staff time for documentation
Risk of repeat tests due to data mismanagement
Digital systems require:
Initial infrastructure investment
Staff training
IT integration
However, long-term benefits may include operational efficiency, scalability, and reduced administrative burden.
When Might Traditional NST Still Be Suitable?
Traditional methods may remain appropriate in:
Low-volume rural centers
Facilities with limited digital infrastructure
Short-term monitoring setups
However, as patient loads increase, scalability becomes a critical consideration.
The Role of Wireless and Portable Fetal Monitoring Devices
Modern systems often include:
Wireless CTG machines
Portable fetal monitors
Integrated uterine contraction monitors
These are particularly beneficial in:
High-dependency obstetric units
Antenatal wards requiring repeated NSTs
Settings requiring mobility and patient comfort
Evidence and Clinical Oversight
While digital tools enhance workflow, it is important to emphasize:
NST interpretation remains clinician-dependent
Technology supports but does not replace obstetric judgment
Proper training is essential for accurate pattern recognition
Hospitals adopting digital NST monitoring must ensure structured implementation, protocol development, and continuous quality review.
Clinical studies available on PubMed (PMID: 3319323, 9475961) support CTG monitoring as a reliable method for tracking fetal wellbeing during pregnancy.
Conclusion: What Should Hospitals Choose?

As maternity units evolve, the shift from paper-based NST systems to digital platforms is becoming less about preference and more about preparedness. While traditional NST machines remain functional, digital NST monitoring offers advantages in centralized oversight, faster escalation, secure documentation, and workflow optimization.
For hospitals looking to adopt a future-ready solution, Keyar Pro Lite is designed to support modern obstetric care with:
Real-time fetal heart rate and uterine contraction tracking
Central monitoring station connectivity
Secure digital data storage
Portable design for flexible bedside use
Clinically reliable performance in high-load labor rooms
Built to enhance clinical visibility without adding operational complexity, Keyar Pro lite supports obstetric teams in making timely, data-informed decisions.
If your hospital is evaluating digital NST solutions, now is the time to assess scalability, integration, and long-term workflow benefits.