Hospitals
How Non-Invasive Bilirubinometers Are Changing the Game? Future of Neonatal Care
Feb 13 • 6 min read

Table of Content
Neonatal jaundice remains one of the most common clinical conditions requiring medical evaluation in newborns. Globally, nearly 60% of term infants and 80% of preterm infants develop jaundice within the first week of life. While most cases are physiological and self-limiting, delayed detection of elevated bilirubin can lead to serious complications including acute bilirubin encephalopathy and kernicterus.
For clinicians and hospital administrators, the challenge is not whether to screen; but how to screen efficiently, safely, and at scale.
How can bilirubin levels be monitored accurately?
How can screening be faster and safer?
How can hospitals reduce laboratory dependency without compromising clinical quality?
The answer increasingly lies in non-invasive bilirubinometers, also known as transcutaneous bilirubin (TcB) devices technology that is redefining neonatal jaundice screening in both NICU and postnatal wards.
Understanding Neonatal Jaundice and Clinical Risk
Bilirubin is a byproduct of hemoglobin breakdown. Newborns are particularly vulnerable to hyperbilirubinemia due to:
Higher red blood cell turnover
Immature liver enzyme systems
Increased enterohepatic circulation
Global health authorities such as the World Health Organization and the American Academy of Pediatrics emphasize that early identification and structured monitoring are critical to prevent neurological injury.
Current AAP recommendations include:
Universal bilirubin screening before discharge
Risk-based follow-up
Plotting bilirubin values on hour-specific nomograms
For busy maternity hospitals, implementing these guidelines efficiently requires rapid, repeatable, and reliable bilirubin measurement.
Limitations of Traditional Serum Bilirubin Testing (TSB)
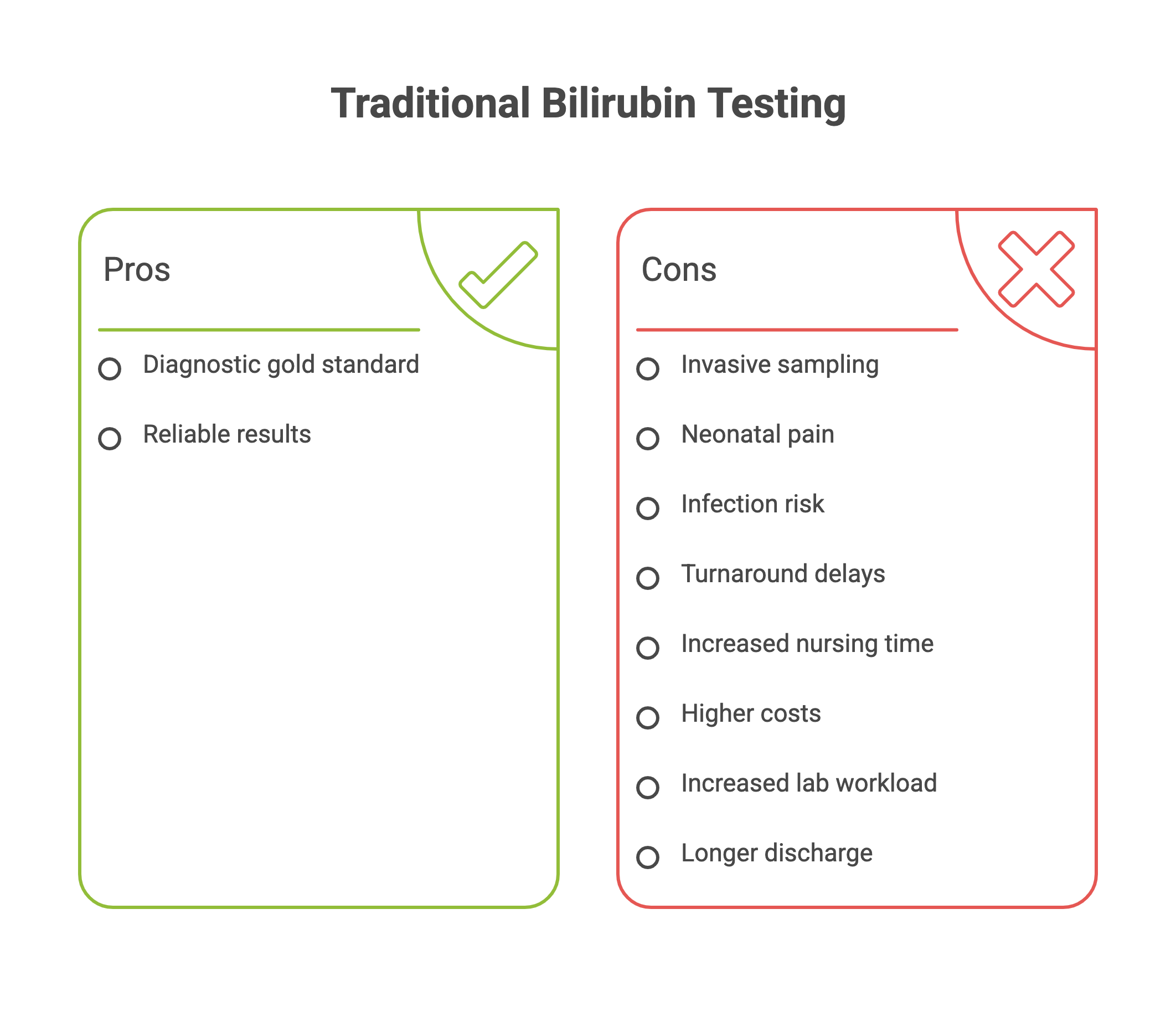
Total Serum Bilirubin (TSB) measurement remains the diagnostic gold standard. However, operationally and clinically, it presents several challenges.
Clinical & Operational Drawbacks
Invasive heel-prick sampling
Neonatal pain and distress
Risk of infection
Turnaround delays due to laboratory workflow
Increased nursing time
Repeated sampling in high-risk infants
For hospital administration, this translates into:
Higher consumable costs
Increased lab workload
Longer discharge timelines
Resource strain in high-delivery-volume settings
As delivery volumes rise, exclusive reliance on laboratory-based bilirubin testing becomes increasingly inefficient. This gap has accelerated the adoption of non-invasive bilirubin monitoring solutions.
What Is a Non-Invasive Bilirubinometer
A non-invasive bilirubinometer measures bilirubin levels transcutaneously (through the skin) without requiring blood sampling.
Also known as a transcutaneous bilirubinometer (TcB), it uses multi-wavelength optical spectroscopy to estimate bilirubin concentration in subcutaneous tissue.
How It Works
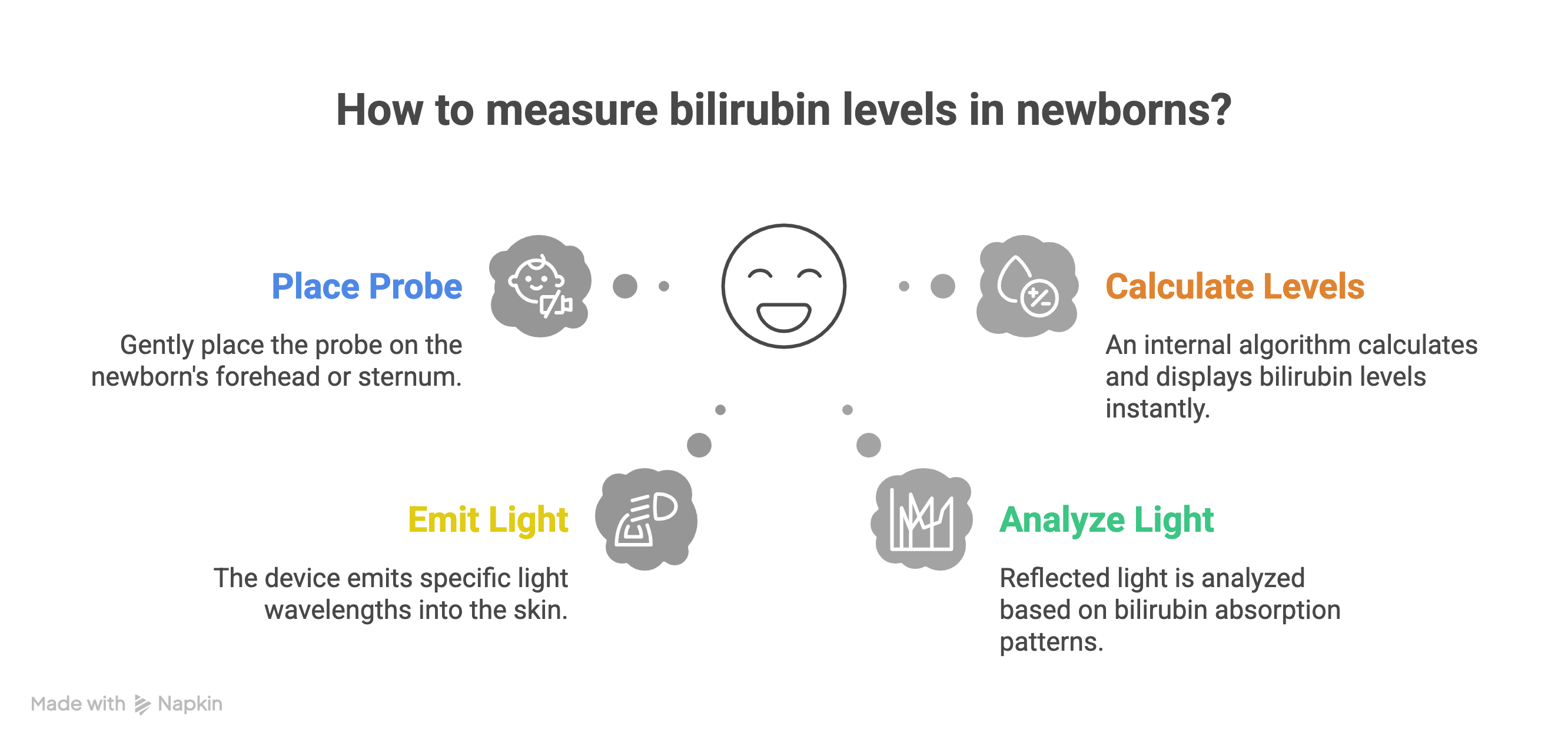
The probe is gently placed on the newborn’s forehead or sternum.
The device emits specific light wavelengths into the skin.
Reflected light is analyzed based on bilirubin absorption patterns.
An internal algorithm calculates and displays bilirubin levels instantly
Results are available within seconds, enabling real-time bedside clinical decision-making.
TcB vs TSB Clinical & Operational Comparison
Effective bilirubin monitoring requires balancing diagnostic accuracy with workflow efficiency. Understanding the difference between TcB and TSB helps clinicians determine when to screen and when to confirm.
Clinical Insight:
While TcB devices are highly effective for screening and trending bilirubin levels, confirmatory TSB testing is recommended when values approach treatment thresholds, as per AAP guidance. This hybrid approach ensures early detection while maintaining clinical safety in treatment decisions.
Clinical Benefits for Doctors
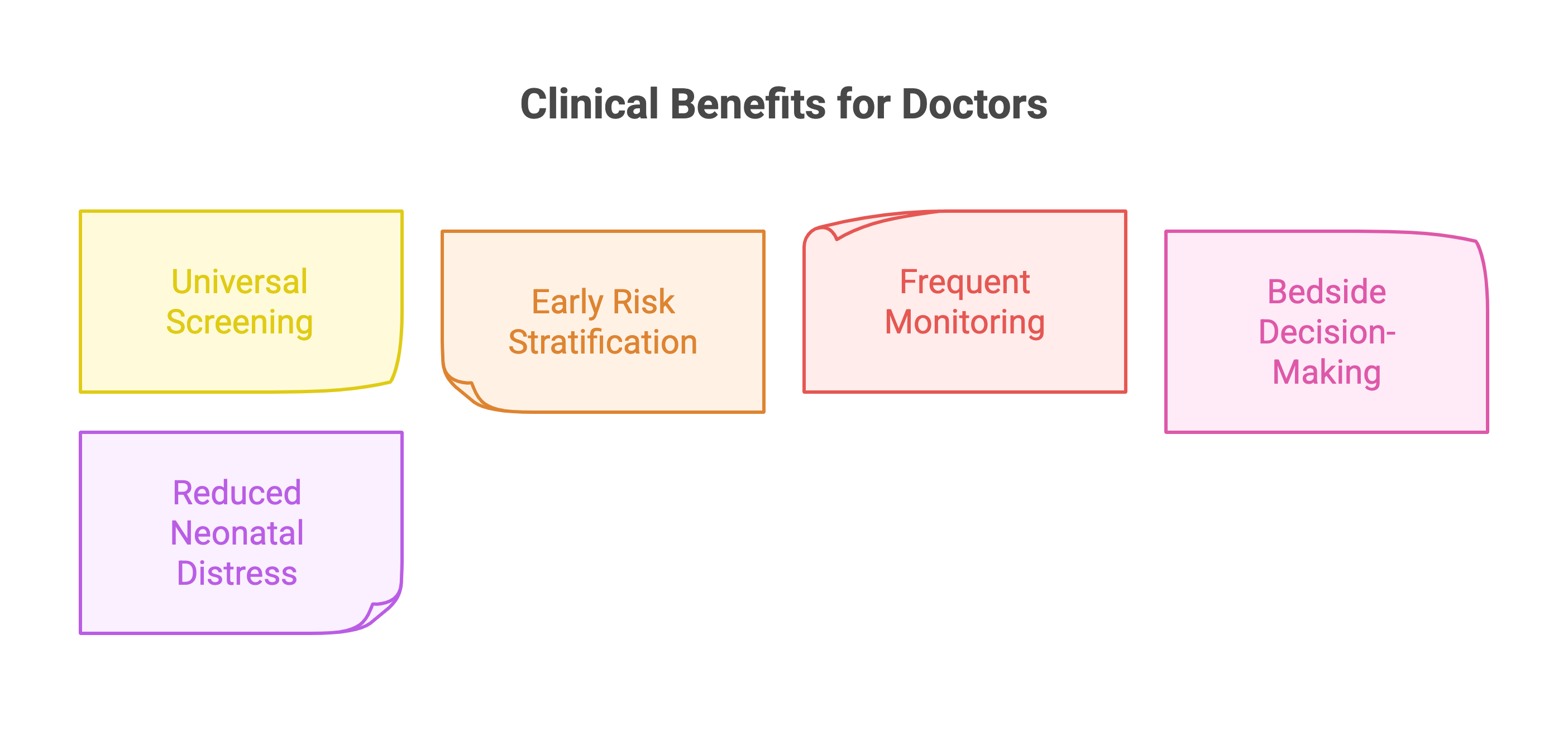
For neonatologists, pediatricians, and obstetric teams, non-invasive bilirubin monitoring enables:
Universal predischarge screening
Early risk stratification
Frequent monitoring of preterm or high-risk infants
Bedside clinical decision-making
Reduced neonatal distress
Repeated monitoring without repeated pricks significantly improves neonatal comfort and strengthens parental confidence.
Operational Benefits for Hospital Administration
Beyond clinical benefits, TcB devices offer measurable operational advantages.
1. Improved Workflow Efficiency
Reduced laboratory dependency
Faster discharge planning
Lower transport and reporting delays
2. Cost Optimization
Reduced consumables (lancets, syringes, lab reagents)
Reduced nursing time per test
Fewer repeat invasive procedures
3. Quality & Accreditation Alignment
Supports compliance with AAP and WHO screening recommendations
Strengthens hospital quality indicators
Enhances patient satisfaction metrics
Hospitals with high delivery volumes particularly benefit from scalable bedside screening solutions.
Accuracy and Clinical Reliabiltiy
Multiple peer-reviewed studies published in journals such as Pediatrics and Journal of Perinatology demonstrate strong correlation between TcB and TSB levels, especially in term and late-preterm infants.
Key considerations include:
Best used for screening and trending
Confirmatory TSB required near phototherapy thresholds
Performance may vary in extremely preterm infants
When integrated into standardized neonatal protocols, TcB devices significantly enhance early detection rates and improve intervention timelines.
The Future Smart Integration & Data-Driven Monitoring
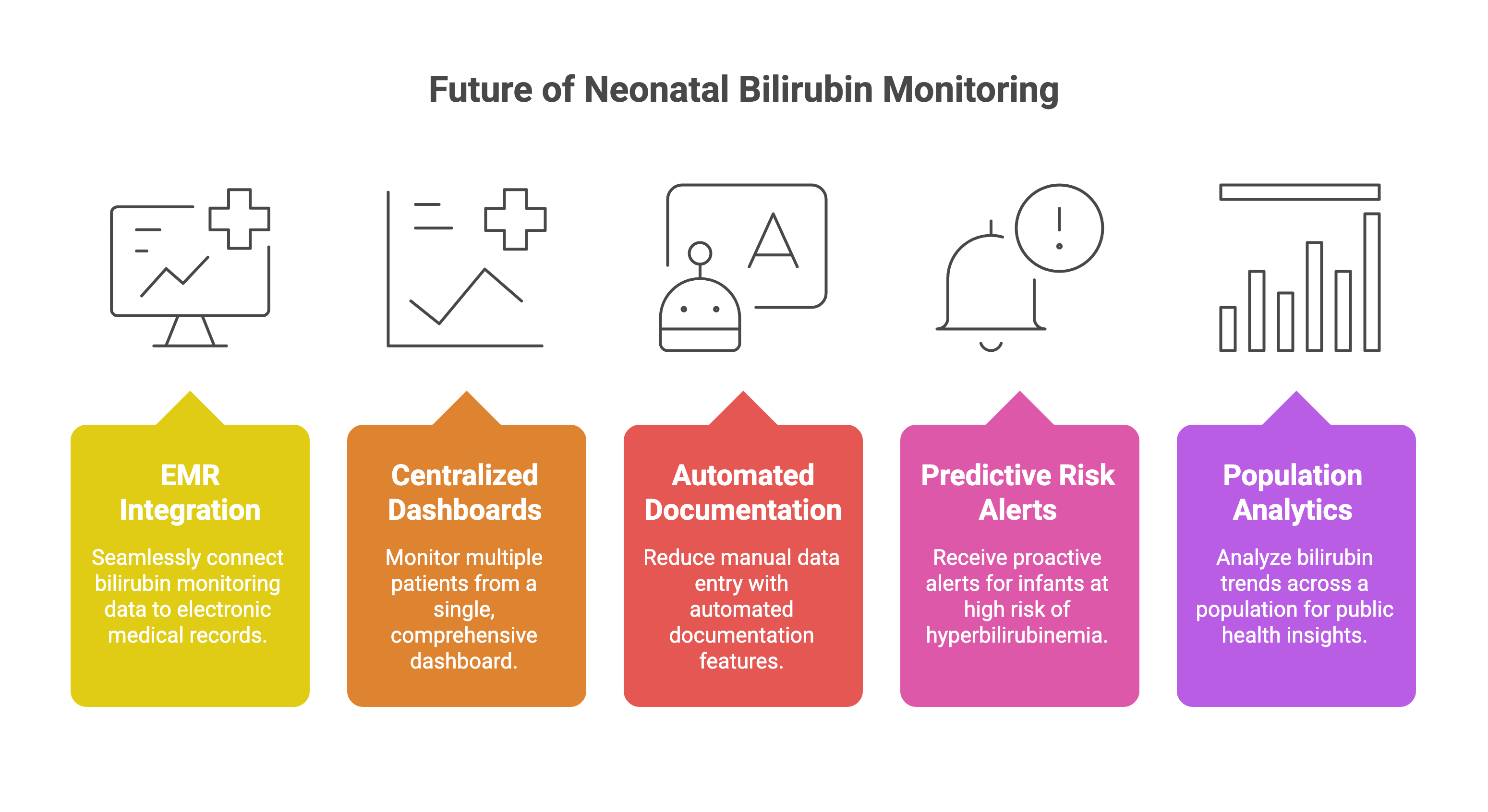
Neonatal bilirubin monitoring is evolving beyond standalone devices. The future includes:
EMR integration
Centralized monitoring dashboards
Automated documentation
Predictive risk alerts
Population-level bilirubin trend analytics
For hospitals investing in digital health infrastructure, integrating TcB devices into centralized maternal and neonatal ecosystems represents the next step in patient safety and care standardization.
Non-Invasive Bilirubin Monitoring by Janitri

To support diverse clinical environments from high-volume tertiary hospitals to digitally integrated maternity centers; Janitri offers advanced non-invasive bilirubin monitoring solutions under the Navam portfolio.
A smart wireless and non-invasive bilirubinometer for quick and painless jaundice monitoring.
Designed for institutional environments requiring centralized visualization and workflow efficiency, Navam Bilirubin Max supports connected neonatal screening.
Key Features:
Portable & easy-to-use
Built-in digital screen
Advanced optical technology
Neonatal bilirubin graph display
Battery-powered device
Remote data access via mobile app
Ideal for NICUs and postnatal wards seeking centralized, scalable bilirubin monitoring.
Navam Bilirubin Pro
Compact wireless and non-invasive bilirubin meter in an aluminum carry case for jaundice monitoring.
Built for portability and flexible deployment, Navam Bilirubin Pro connects easily to the JFH mobile app using a smartphone, enabling streamlined bedside screening.
Key Features:
Portable & easy-to-use
Built-in digital screen
Optical spectroscopy technology
Neonate bilirubin graph display
Battery-powered device
Remote data access via mobile app
Navam Bilirubin Pro supports efficient predischarge screening and repeat monitoring without increasing laboratory burden.
Conclusion
As neonatal care shifts toward gentler, evidence-based practices, non-invasive bilirubin screening is rapidly becoming a standard of care rather than an alternative. Transcutaneous bilirubinometry enables early detection, confident trend monitoring, and reduced reliance on invasive blood sampling; without compromising clinical accuracy.
By integrating advanced TcB solutions like the Navam portfolio, hospitals can enhance neonatal safety, streamline workflows, and align with global screening recommendations.
Book a demo today to explore how Janitri’s non-invasive bilirubin monitoring solutions can elevate your maternity workflow and redefine newborn jaundice screening standards.
FAQ’s
What instrument is used to measure bilirubin?
Bilirubin is measured using a bilirubinometer in laboratories or a transcutaneous bilirubinometer (TcB) for non-invasive screening. Laboratories use automated chemistry analyzers to measure serum bilirubin levels accurately from a collected blood sample.
What are the methods of measuring bilirubin?
Bilirubin is measured using two main methods: a serum bilirubin blood test and a transcutaneous bilirubin (TcB) skin test. The blood test provides detailed results, while TcB offers quick, non-invasive screening in newborns.
Which method is best for bilirubin test?
The serum bilirubin blood test is considered the gold standard because it provides precise total and direct bilirubin levels. It is most reliable for diagnosis and treatment decisions, especially when jaundice levels are high.
What is a non-invasive test for jaundice?
The transcutaneous bilirubin (TcB) test is a non-invasive method for detecting jaundice. A handheld device is placed on the baby’s skin to estimate bilirubin levels without drawing blood, making it safe and painless.
How accurate is a bilirubinometer?
Laboratory bilirubin testing is highly accurate and used for clinical decisions. Transcutaneous bilirinometers are reliable for screening and usually correlate closely with blood results, but high readings should be confirmed with a serum test.
References
Shabuj MH, Hossain J, Dey S. Accuracy of transcutaneous bilirubinometry in preterm infants: a comprehensive meta-analysis. J Matern Fetal Neonatal Med. 2019;32(5):734-741. PMID: 28992717.
Lucanova LC, Matasova K, Zibolen M, Krcho P. Accuracy of transcutaneous bilirubin measurement in newborns after phototherapy. J Perinatol. 2016;36(10):858-861. PMID: 27279078.