Hospitals
Why Visual Assessment of Jaundice Can Be Misleading in Newborns?
Mar 27 • 9 min read

Table of Content
vEvery year, millions of newborns develop jaundice, a yellowing of the skin and eyes caused by elevated bilirubin levels in the blood. While jaundice in newborns is often harmless and self-resolving, severe, untreated hyperbilirubinemia in newborns can cause permanent neurological damage or death. The challenge? One of the most commonly used tools to detect it, the human eye, is dangerously unreliable.
In this blog, we explore why visual assessment of jaundice in the newborn can lead to missed diagnoses, the gold standard for accurate bilirubin testing, and why modern tools like a transcutaneous bilirubinometer or non-invasive bilirubin test device are transforming neonatal care worldwide, including in India.
Understanding Jaundice in the Newborn
Jaundice happens when bilirubin, a yellow pigment that the body naturally produces as it breaks down old red blood cells, builds up faster than the liver can clear it out. In newborns, this is actually very common. Their livers are still finding their footing in those first few days of life, and on top of that, their bodies are breaking down red blood cells at a much faster rate than adults. So it is really no surprise that so many babies end up with some degree of jaundice shortly after birth.
The causes of neonatal jaundice include:
• Physiological jaundice — appears 2–4 days after birth, typically resolves within 1–2 weeks
• ABO or Rh blood group incompatibility between mother and baby
• Breastfeeding jaundice due to inadequate milk intake in the first days of life
• Breast milk jaundice — longer-lasting but generally benign
• G6PD deficiency — common in South Asian, African, and Mediterranean populations
• Infections and sepsis
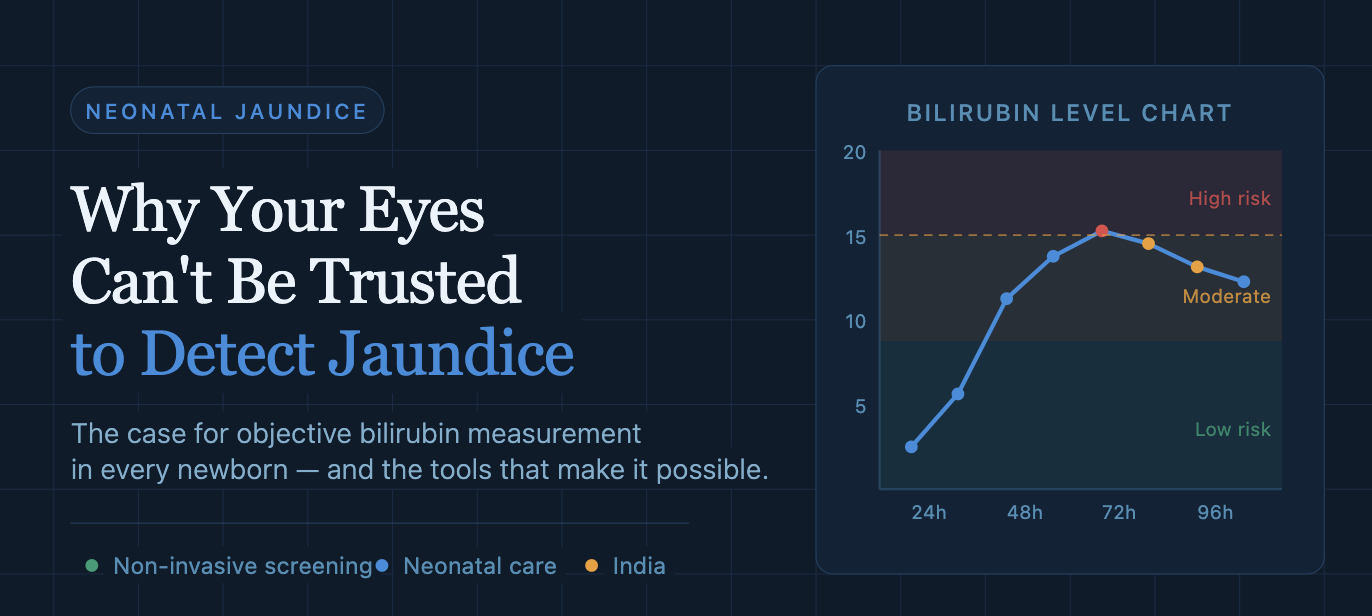
Understanding the bilirubin level chart and tracking bilirubin in neonates over time is essential. The normal bilirubin level in newborn infants varies by age in hours and by risk factors. What appears normal at 24 hours may be dangerously elevated at 72 hours — which is exactly why a single visual check is insufficient.
The Problem with Visual Assessment: Why Clinicians Can Be Fooled?
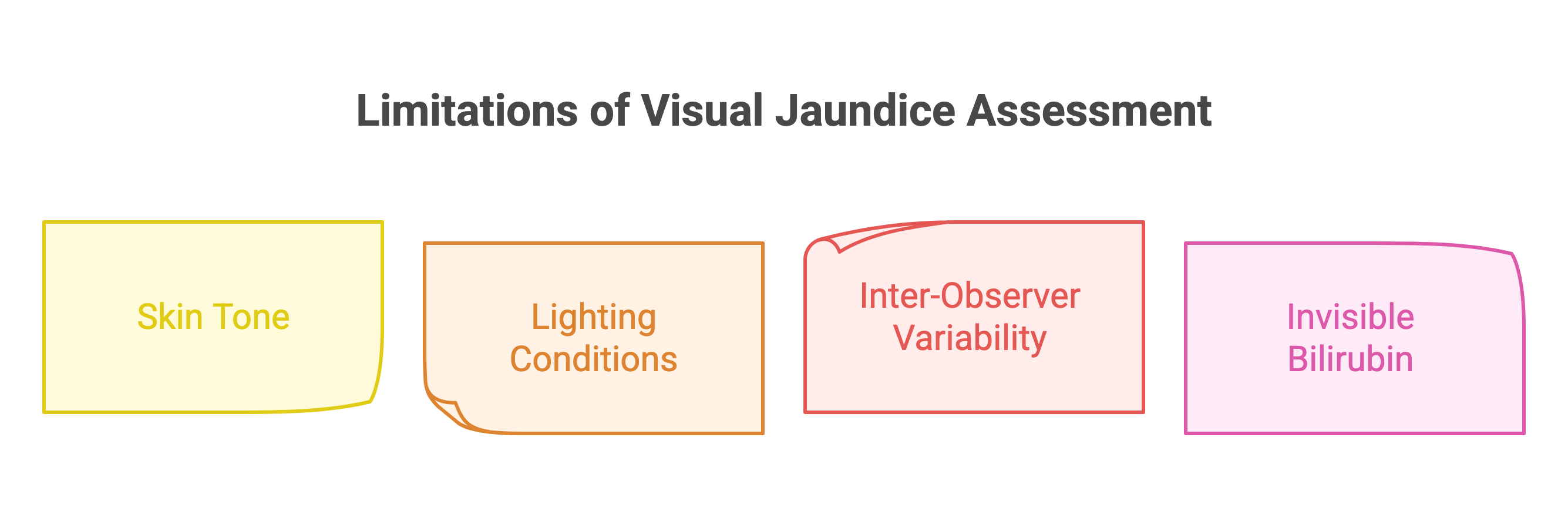
For decades, clinicians have relied on visual inspection, pressing the skin to blanch it and observing the yellow tinge underneath, as a first-line jaundice screening method. However, growing clinical evidence reveals that visual assessment is subject to significant and potentially dangerous error.
1. Skin Tone Masks Jaundice Severity
The most well-documented limitation is the effect of skin pigmentation. In darker-skinned newborns, common across South Asian, African, and Hispanic populations, the yellow discolouration of jaundice is significantly harder to detect visually. A baby with severe hyperbilirubinemia in a newborn may appear only mildly yellow to the naked eye, leading clinicians and parents alike to underestimate the risk. In fairer-skinned babies, the reverse can occur: a healthy yellow tint from carotenoids in breast milk may be mistaken for clinical jaundice.
2. Lighting Conditions Distort Colour Perception
Hospital wards often use fluorescent or LED lighting that alters the perceived colour of skin. Clinical studies have demonstrated that even trained neonatologists significantly underestimate bilirubin levels under artificial lighting. In natural daylight, assessments may differ entirely. Since postnatal wards are rarely lit consistently, this variability introduces a dangerous element of chance into jaundice screening.
3. High Inter-Observer Variability
Different clinicians examining the same baby can arrive at entirely different conclusions about jaundice severity. Research shows inter-observer agreement on visual jaundice grading is consistently poor, even among experienced professionals. The Kramer scale, which maps jaundice progression from the face down to the extremities, correlates loosely with actual serum bilirubin levels and cannot be used reliably in isolation.
4. Bilirubin Builds Invisibly Below the Surface
Bilirubin deposits in tissues at a rate that does not always correlate with visible skin changes. A newborn can have significantly elevated bilirubin in infants without displaying the classic head-to-toe yellowing that clinicians are trained to identify. By the time visible signs become pronounced, bilirubin levels may have already crossed dangerous thresholds requiring urgent intervention.
Symptoms of Jaundice in Newborns: Beyond the Yellow Skin
The symptoms of jaundice in newborns extend well beyond skin colour and include:
• Yellow tinge to the whites of the eyes (scleral icterus)
• Dark yellow urine and pale or chalky stools
• Lethargy, poor feeding, and difficulty waking
• High-pitched cry; a warning sign of acute bilirubin encephalopathy
• Arching of the back (opisthotonus) in severe cases
None of these symptoms provide an accurate measure of bilirubin levels. They serve only as red flags that prompt further investigation, specifically, a formal bilirubin test.
How Is a Bilirubin Test Done?
There are two primary methods for measuring bilirubin levels in newborns:
Serum Bilirubin Test (Blood Test)
The traditional gold standard involves drawing blood either from a heel prick or venipuncture, and sending the sample to a laboratory for total serum bilirubin (TSB) analysis. While highly accurate, it is invasive, time-consuming, painful for the neonate, and requires laboratory infrastructure. Repeated sampling is necessary for monitoring compounds; all these disadvantages significantly.
Non-Invasive Bilirubin Test (Transcutaneous Method)
A transcutaneous bilirubin device, also called a bilirubinometer or transcutaneous bilirubinometer uses multi-wavelength spectrophotometry to estimate bilirubin levels through the skin. A probe is gently pressed against the baby's forehead or sternum, and within seconds, a reading is displayed on the screen. The non-invasive bilirubin test is painless, immediate, and requires no blood draw, making it ideal for routine jaundice screening device applications in any setting.
Transcutaneous vs Blood Bilirubin Test: Which Is Better for Newborn Jaundice Screening?
The debate between transcutaneous vs blood bilirubin test methods has been central to neonatal medicine for two decades. Here is what current clinical evidence tells us:
Parameter | Transcutaneous (TcB) | Serum (TSB – Blood) |
Invasiveness | Non-invasive | Invasive (heel prick) |
Pain to Neonate | None | Yes |
Result Time | Seconds | 30–60 minutes (lab) |
Accuracy | High (~±2–3 mg/dL) | Highest (gold standard) |
Cost per Test | Low (device reuse) | Moderate (lab reagents) |
During Phototherapy | Less reliable | Accurate always |
Best Use | Screening & monitoring | Confirmation & treatment |
Clinical guidelines from the American Academy of Pediatrics (AAP) and the National Institute for Health and Care Excellence (NICE) both recognise transcutaneous bilirubinometry as an appropriate first-line screening tool, with serum testing reserved for confirming borderline or high-risk readings. Many leading Indian neonatal units have adopted the neonatal bilirubin device as standard protocol, reducing unnecessary blood draws, improving throughput, and enhancing the experience for families.
Newborn High Bilirubin Treatment: What Happens When Levels Are Elevated?
When bilirubin in infants treatment becomes necessary, the approach depends on severity and gestational age:
• Phototherapy: The most common newborn high bilirubin treatment. Specific wavelengths of blue-green light (460–490 nm) convert bilirubin into water-soluble forms that can be excreted without hepatic conjugation.
• Intensive phototherapy or exchange transfusion: Reserved for extremely high levels or when standard therapy fails.
• Treating underlying causes: Managing haemolytic disease, treating infection, or supplementing breastfeeding.
• Ongoing monitoring with a bilirubin device for newborn: Regular transcutaneous or serum checks to track treatment response and guide discharge decisions.
Accurate bilirubin measurement is not just diagnostic; it is the cornerstone of safe treatment. Phototherapy thresholds, discharge criteria, and follow-up intervals are all determined by objective bilirubin values plotted on standardised bilirubin level charts. A subjective visual estimate cannot and should not guide these critical clinical decisions.
Choosing a Bilirubinometer in India: What Hospitals and Clinics Need to Know
For hospitals and clinics looking to buy a bilirubin device in India, several important considerations apply:
Hospital Grade vs Basic Devices
A hospital-grade bilirubinometer offers higher accuracy, validated clinical performance across diverse skin tones, and connectivity for data logging and EMR integration. These features are essential in NICUs and tertiary care settings. Entry-level devices may suffice for community screening in primary health centres, but should always be locally validated before clinical adoption.
Transcutaneous Bilirubinometer Price in India
The transcutaneous bilirubinometer price in India varies based on brand, technology, and features. Entry-level devices may start at approximately ₹80,000–₹1,20,000, while advanced hospital-grade bilirubinometer models with data connectivity can range from ₹1,50,000 to ₹3,00,000 or more. When evaluating bilirubinometer price in India, hospitals should factor in the total cost of ownership: the device, calibration accessories, consumable probe tips (if applicable), service contracts, and staff training. A higher upfront cost is often offset by savings from reduced blood draws and laboratory costs.
Key Features to Look for in a Bilirubin Device for Newborns
• Clinically validated across diverse skin tones — critical for Indian patient populations
• Wide measurement range (typically 0–25 mg/dL) to cover high-risk neonates
• Ergonomic, one-handed operation suitable for ward nurses
• Built-in memory and data export capability for EMR integration
• Regulatory approval: CE marking, FDA clearance, or CDSCO registration in India
When you buy a bilirubin device for your facility, always request the clinical validation data specific to the model and confirm appropriate regulatory certification for the Indian market.
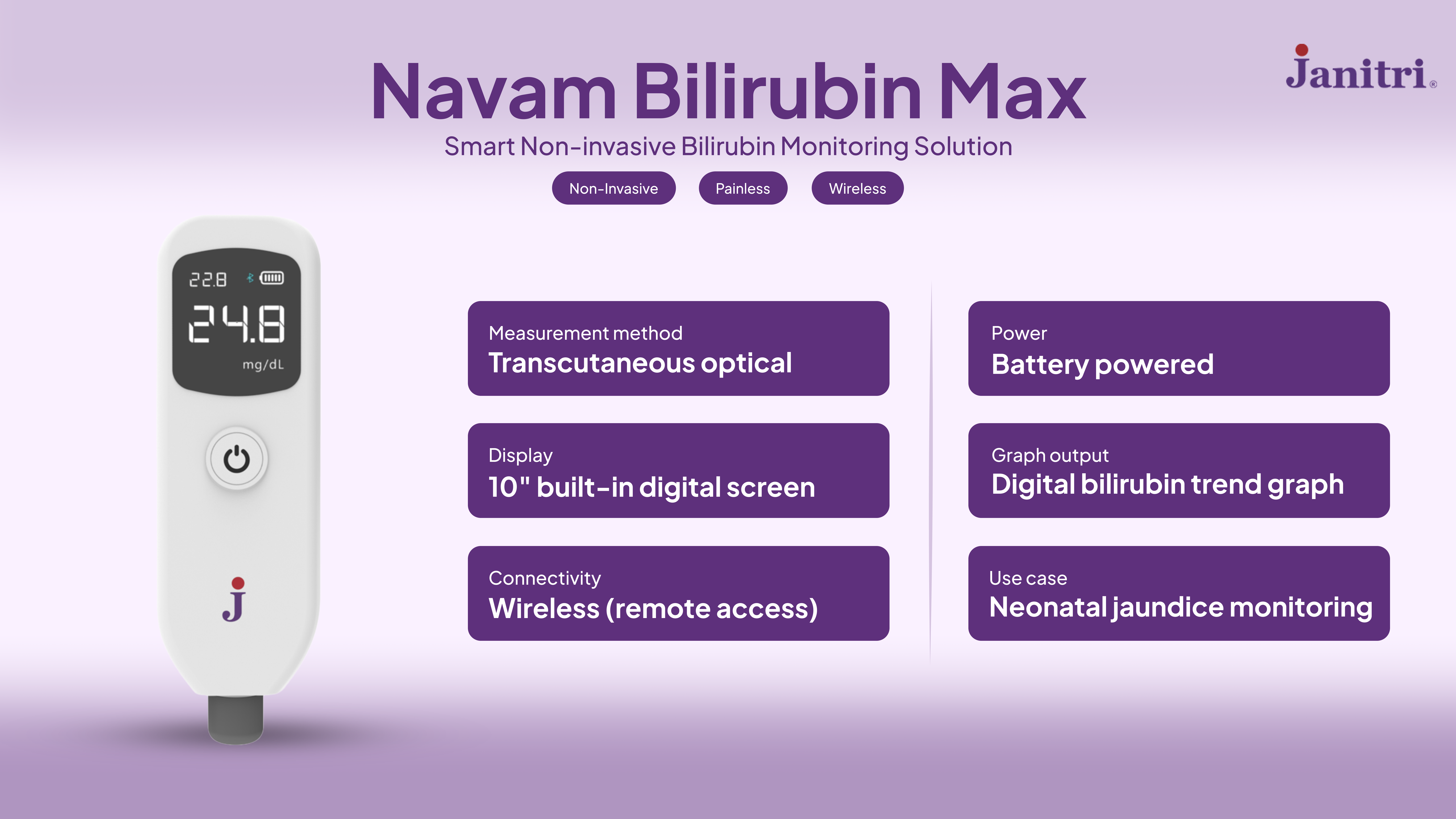
Introducing Non-Invasive Bilirubin Meter: Navam Bilirubin Pro
Navam Bilirubin Pro is a non-invasive transcutaneous bilirubin monitoring device designed for quick, accurate, and painless jaundice screening.
Non-invasive means it measures bilirubin levels through the baby’s skin without needles or blood draws, making it safe, painless, and ideal for frequent monitoring.
Unlike visual assessment, which can be affected by skin tone, lighting conditions, and human judgment, Navam Bilirubin Pro provides objective, numeric bilirubin values. Visual screening often misses early or rising bilirubin levels and cannot accurately track trends over time; critical parameters needed for timely intervention.
Built for hospitals and clinical settings, it enables healthcare professionals to make faster, more accurate, and data-driven decisions in newborn care.
Why Navam Bilirubin Pro?
Non-invasive & painless
Eliminates the need for heel pricks, reducing stress for both newborns and parents.Instant results
Provides bilirubin readings within seconds, enabling immediate clinical decisions.Designed for Indian skin tones
Clinically reliable across diverse pigmentation, addressing one of the biggest limitations of visual assessment.Ideal for routine screening & monitoring
Supports early detection and continuous tracking, reducing the risk of missed hyperbilirubinemia.User-friendly & efficient
Ergonomic design allows easy use by nurses and clinicians in busy neonatal units.
Bridging the Gap Between Screening and Safety
As highlighted earlier, objective bilirubin measurement is the cornerstone of safe neonatal care, not visual estimation alone. Navam Bilirubin Pro helps bridge this gap by making accurate screening accessible, fast, and repeatable, ultimately improving outcomes and reducing unnecessary invasive testing.
Conclusion
Neonatal jaundice is a near-universal occurrence, but jaundice that progresses to kernicterus is a preventable tragedy. The gap between these two outcomes is often a matter of accurate, timely bilirubin measurement.
Visual assessment, while useful as an initial prompt, consistently fails as a standalone clinical tool. Skin tone variation, inconsistent lighting, inter-observer disagreement, and the absence of a reliable linear relationship between skin colour and bilirubin level all render it inadequate for informed clinical decision-making.
The evidence is clear: every newborn deserves objective jaundice screening. For hospitals and clinics, deploying a validated non-invasive bilirubin test system, a transcutaneous bilirubin device or bilirubinometer, as standard of care significantly reduces the risk of missed hyperbilirubinemia, unnecessary blood draws, and costly complications.
As neonatal care standards rise across India and globally, investing in a reliable bilirubin device for newborn screening is not just a clinical decision. It is a commitment to the safest possible start in life for every baby born in your care.